What is attention deficit disorder?

"Attention deficit disorder" or ADD used to be a frequently used term in the United States. However, since the late 1980s it has fallen out of favor and been subsumed under the umbrella term "attention deficit hyperactivity disorder" or ADHD. Both ADD and ADHD describe learning difficulties related to attention, the difference is mainly the hyperactivity and impulsivity that some children and adults experience.
To accommodate attention deficit disorder under attention deficit hyperactivity disorder, ADHD is described as having different presentations 1) primarily inattentive, which corresponds to ADD, 2) impulsive and hyperactive, or 3) a combined presentation.
Depending on the source you are consulting, you’ll find ADHD can be written AD/HD, ADD/ ADHD or AD(H)D or even still ADD. Are you confused yet? Even more befuddling is that ADD is still sometimes used in the UK.
In this article, we primarily use the umbrella term ADHD to discuss attention deficit disorder with and without hyperactivity.
ADHD as a specific learning difficulty
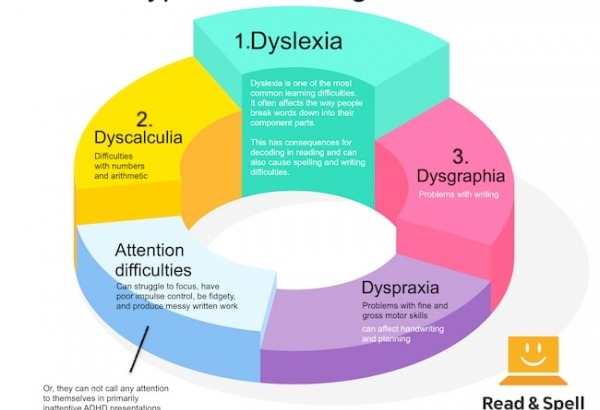
Children and adults with ADHD have things in common with individuals who have other specific learning difficulties, such as dyslexia, dyscalculia, and dyspraxia, particularly when it comes to looking at how they learn best. A specific learning difficulty can range from mild to severe in its impact, and is not related to an individual’s health, intelligence, educational, intellectual or social potential (nor is it related to cultural or class background). The key word here is potential.
Each of the aforementioned specific learning difficulties can introduce its own set of sometimes overlapping challenges to be overcome if an individual is to learn, thrive and achieve success in various aspects of life. But for children with ADHD, as well as for their teachers and parents, this can sometimes be hard work. Strategies and skills for success need to be understood, learned and applied and strengths recognized to ensure motivation and self-esteem remain high.
Thankfully, knowledge, understanding and support from parents and teachers can make a world of difference. To succeed students, teachers and parents need to be aware of how aspects and symptoms of a child's ADHD affect him or her differently. They need to look at how treatment may affect physical and mental health and well-being, and how specifically selected responses and strategies can facilitate behavior management and support optimal performance and achievement at school.

Diagnosis and symptoms
There is no definitive test to assess if someone has ADHD. It is believed that neurobiological, genetic and environmental causal factors can all be involved, and there are still differences of opinion on how to approach diagnosis and treatment (3, 4, 5). Issues around ADHD treatment, particularly medication are controversial in the health and education sectors and differ from country to country. But there is not much doubt that ADHD is now accepted as a neuro-developmental psychiatric disorder and that for some, medication has a place in its remediation.
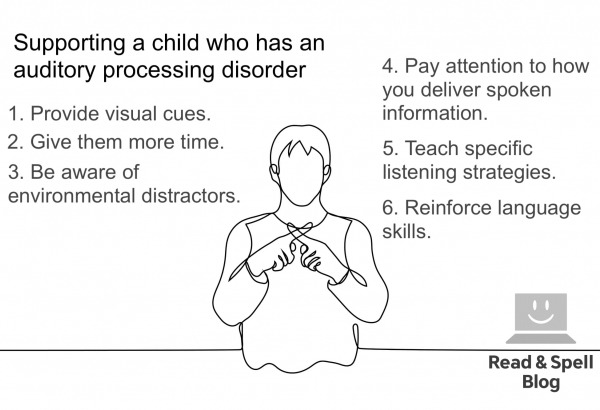
A number of concerning behaviors attributed to ADHD can also fall within what is considered to be the normal range and it’s not always easy to tell if a child has ADHD without a proper professional diagnosis. In very young school age children, some behaviors are entirely consistent with early developmental delays. Also, auditory perception symptoms can look a lot like ADHD, so it’s important to ascertain that the difficulty is attention rather than perception. Learn more about recognizing an auditory processing disorder in children with ADHD.
A diagnosis involves many factors including that the concerning behaviors have lasted for a significant period of time, which may begin before the child started primary school, but certainly by the time the child is twelve. It's also interesting to note that it's been speculated children with ADHD who do not have symptoms of hyperactivity or impulsivity – particularly girls - are under-diagnosed and therefore at a higher risk for academic failure. This is because their symptoms may be less visible in the classroom.
Primarily inattentive presentations of ADHD can look like this
Symptoms may be mild or severe but for illustrative purposes, the descriptions given below are extreme:
The student sits there quietly, distracted and unfocused, and fails. Their self-esteem is compromised, so they fail again, and it becomes a downward spiral. They have poor social adjustment and behavioral problems, not in the ADHD hyperactive way, but by disengaging and not paying attention.
They are easily frustrated because they are not really sure what’s going on around them. It’s hard on them if, for example, suddenly everyone is laughing and they don’t know why; it can be alienating, stressful as well as tiring, and it’s not surprising they might start to act out or that their mental health may suffer.
A note for teachers
Without appropriate interventions, a long-term consequence of extreme inattentive presentations of ADHD, formerly called ADD, can be children dropping out of school, delinquency and substance abuse. If you are a teacher who suspects that a child in your class has undiagnosed ADHD, you could consider undertaking focused observations in a variety of school settings. Observe the child in English and gym or physical education class for contrast. Sit in on their art and music lessons (students with ADHD are often quite creative!) watch them during independent study and have a look at their notes from science and history class.
Take notes on the symptoms you observe. Sometimes this is something observers fail to do, but you know the symptoms you are looking for. These notes will be invaluable when it comes time to discuss the child with the parent, ask for a classroom observation by a specialist, or refer the child for assessment and or help them find treatment.
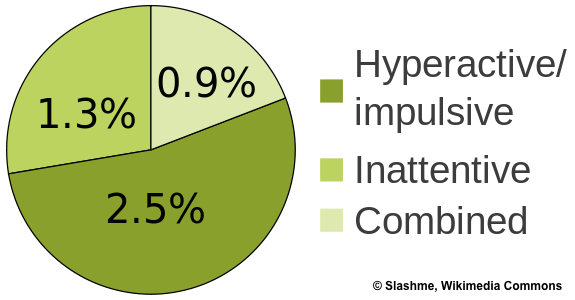
Incidences of ADHD
In 2013, the World Health Organization recognized ADHD as the most common psychiatric disorder in children and young adults, estimating it affects more than 38 million people (6). It is not known why someone develops ADHD, but it has been more commonly observed in boys than girls (7, 8).
Symptoms of inattentive presentations of ADHD and how to help
According to the definition we are using, children with inattentive ADHD, formerly known as ADD, have attention deficits without the hyperactivity. They are likely passive and don’t bother anyone. They can be like-able, but are often rejected by their peers as there’s not much happening around them.
If a child has difficulty making and keeping friends or struggles to engage in social behavior, it might help to get them to show another child how to do something, or pair them up with a peer to undertake an activity. You might also allow them to demonstrate something they’ve accomplished to the whole class, even perhaps letting them show off a little as this is a positive behavior and these might be children who receive a disproportionate amount of negative recognition in academic environments.
Children with inattentive presentations of ADHD may come across as timid and ineffectual, or phased out, as if in a daze. They can be quiet and laid back. Particularly in a disruptive class, they may disappear into the background and be overlooked for attention. They won’t necessarily ask for help, and you may have to go to them to initiate it and start to build up a calm and supportive relationship.
The child with inattentive ADHD doesn’t always concentrate, and because of this lack of focus, their comprehension may be poor. They may not complete or turn in their work. They can have impulsivity in a different way to the child with ADHD. It may be more subtle. They may not want to delay gratification, but they can lack focus.
These are children who have trouble getting started on assignments even if they understand what they have to do, so you might have to help them to get going.
More tips for teachers
They may put their hand up with a question without first thinking the assignment through and deciding how to proceed. This can apply to a lot of children, not only those with ADHD. Sometimes they may start an assignment without understanding what they should be doing – here’s that impulsivity kicking in again.
These are children who tend to focus on trivia and might perseverate on a small and insignificant item without getting the big picture. Or alternatively, some will get the big picture but can’t focus on the details. Integration of new learning with what children with ADHD already know can be a problem, and this becomes more apparent as they get older.
So what you might see is that they have discrete bits of information, but they don’t get the whole concept because they haven’t paid enough attention to be able to hang them together.
Children with ADHD might quickly become bored. It's possible that they don’t always listen, can be forgetful, lose things, are not prepared, or not able to find their homework. They might generally seem disorganized and easily distracted by movement, noise, and other things that are happening around them.

Helping them stay organized
One of the best things you can do for a student or child with ADHD is to help them stay organized. How you go about this is important.
Reminding them to bring their pencil next time if they always forget might not be the best approach. In fact, it can be annoying and ineffective for both the child and the teacher. Consider the student who has forgotten their pencil again and knows they are going to get into trouble and other children are likely to laugh. This can be a trigger for a bit of acting out.
Instead, have a basket of pencils available for them or create a set of reminder cards they can review before coming to their lesson and make one for "bring a pencil." Look into adding a special pencil case that attaches to their bag, or even a pencil on a keychain that they can always have with them. If the forgotten item is something larger, like a workbook which goes back and forth to the home, consider working with their parents to institute a routine related to preparing their bag for school.
For children with specific learning difficulties, the teacher has to think in terms of adaptations vs. rules. Children with ADHD also need strong and clear directions and ample praise when they get something right.
Treatment in the classroom
To help a child manage their ADHD, you want the least possible stimuli around them. It’s advised that you don’t sit them near a window, a heater or a high traffic area. Children who don't have ADHD might not be bothered by these things, but for students with ADHD, even small distractions can lead to a loss of attention and focus. A child with ADHD can benefit from a stimulus reduced study area both at home and at school.
Keep in mind they may struggle to handle surprises, such as a visitor to the class or the fire alarm going off. It can help to get them settled in a seat they're going to have for the full year. Teachers may also designate the same seat in a computer lab. This is because the child may have difficulty with transitions and relocations.
A child with ADHD may be able to watch television or play computer games for hours on end – the key being that these are activities they enjoy - but they can’t focus at school, have a short attention span and are easily bored. They may have difficulty processing new information at speed. They may work slowly, move slowly and need extra time.
The child may also have poor fine motor skills, and produce messy work, symptoms similar to children who struggle with handwriting difficulties and dyspraxia.
More ways to help
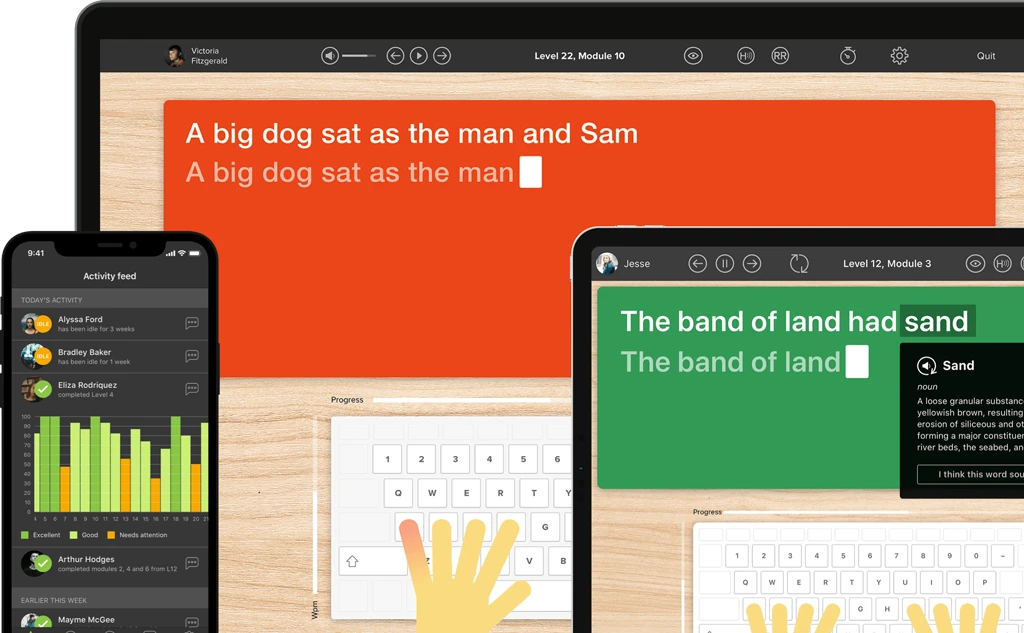
Many teachers and parents find Touch-type Read and Spell is both popular and effective with children who have ADHD. It teaches them typing skills using a unique, ADHD-friendly approach, and strengthens reading, writing and spelling skills at the same time.
TTRS is designed to make students feel and be successful, which inevitably helps improve mental health and self-esteem and motivates them to go on. It is highly structured, delivers information in a multi-sensory way in small incremental steps, and learners work at their own pace and with as much repetition as they need.
The use of headphones for the audio helps students screen out distractions. Children may not understand percentages of success, but can see how well they are doing on a big red bar graph. The course can be used for children aged seven and up, once the hands are mature enough to sit comfortably on a keyboard.
References
1) Weiss, Lawrence G. (2005). WISC-IV clinical use and interpretation scientist-practitioner perspectives (1st ed.). Amsterdam: Elsevier Academic Press. p. 237. ISBN 9780125649315.
2) Parrillo, V.N. (2008). Encyclopedia of Social Problems. SAGE. p. 63. ISBN 9781412941655.
3) Sim, M.G., Hulse, G., Khong, E. (2004). When the child with ADHD grows up. Aust Fam Physician 33 (8): 615–618. PMID 15373378.
4) Silver, L.B. (2004). Attention-deficit/hyperactivity disorder (3rd ed.). American Psychiatric Publishing. pp. 4–7. ISBN 9781585621316.
5) Schonwald, A., Lechner, E. (2006). Attention deficit/hyperactivity disorder: complexities and controversies. Curr. Opin. Pediatr. 18 (2): 189–195.
6) Cowen, P., Harrison, P., Burns, T. (2012). Shorter Oxford Textbook of Psychiatry (6th ed.). Oxford University Press. p. 546.
7) Kooij, S.J., Bejerot, S., Blackwell, A., Caci, H. et al. (2010). European consensus statement on diagnosis and treatment of adult ADHD: The European Network Adult ADHD. BMC Psychiatry 10: 67.
8) Bálint, S., Czobor, P., Mészáros, A., Simon, V. et al. (2008). Neuropszichológiai károsodásokat felnőtt figyelemhiányos hiperaktivitás zavar(ADHD): A szakirodalmi áttekintés [Neuropsychological impairments in adult attention deficit hyperactivity disorder: A literature review]. Psychiatria Hungarica (in Hungarian) 23 (5): 324–335. PMID 19129549.
For learners who struggle with attention difficulties
TTRS is a program designed to get children and adults with attention difficulties touch-typing, with additional support for reading and spelling.
Meredith Cicerchia

close
Can an Orton-Gillingham approach to literacy help your child?
Take a short quiz to find out!
TTRS has a solution for you
An award-winning, multi-sensory course that teaches typing, reading and spelling
How does TTRS work?
Developed in line with language and education research
Teaches typing using a multi-sensory approach
The course is modular in design and easy to navigate
Includes school and personal interest subjects
Positive feedback and positive reinforcement
Reporting features help you monitor usage and progress